Genetic Counseling
Genetic counseling provides individuals and families with information regarding genetic conditions including how the condition is passed down in a family (inheritance), and the symptoms of the condition (how it may affect a person). Having this information can help patients and families make informed medical and personal decisions. The next section reviews genetic risk assessment and the use of family history and genetic testing to diagnose genetic conditions. This section does not address all personal, cultural, or ethical issues that individuals may face, nor does it substitute for speaking with a genetics professional. To find a genetics or prenatal diagnosis clinic, see the GeneTests Clinic Directory.
A Brief Lesson in Genetics
Genes are the instruction manual for our bodies. They are made up of DNA and packaged in chromosomes. Usually people have 46 chromosomes in every cell. Cells are the building blocks of the body. In almost all cells, the 46 chromosomes are present in 23 pairs. One chromosome from each pair comes from the father, and one comes from the mother. This is why a child resembles the entire family.
When we look at the 23 pairs of chromosomes, there are some differences. The first 22 pairs carry most of the information (genes) that makes us who we are. The 22nd chromosome is the smallest. The 23rd pair are the sex chromosomes and determine if a person is male or female.
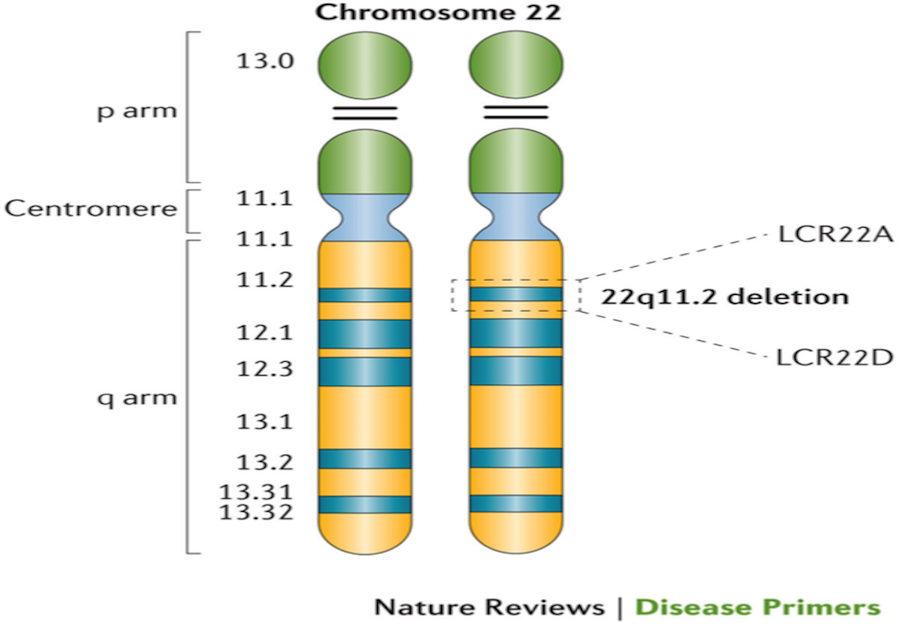
McDonald-McGinn, D. M. et al. (2015) 22q11.2 deletion syndrome
Nat. Rev. Dis. Primers doi:10.1038/nrdp.2015.71
If a person has the 22q11.2 deletion syndrome this means that a small amount of information (about 50 genes) is missing or deleted from the 22nd chromosome. Because the deletion is so small, a special test is needed to make this diagnosis. The 22q11.2 deletion is present from the moment that the mother’s egg and the father’s sperm come together to make a baby. There is nothing that the parents did or did not do that caused the 22q11.2 deletion to happen. It is not due to illnesses, medications, food, drink, cigarettes, or drugs used by the parents before, during or after the pregnancy. In most families, the 22q11.2 deletion is a new condition and no one else in the family is affected.
However, in about one in ten families (or 10%) the 22q11.2 deletion is found in either the mother or the father. In these cases, the deletion is inherited. Because of this chance, it is recommended that both parents be tested for the 22q11.2 deletion when they have a child with this condition. Knowing if the 22q11.2 deletion is inherited is important. Parents with the deletion may need additional medical care for themselves and they have a 50% (or 1 in 2) chance of having another child with the deletion in all future pregnancies.

One out of ten families who have a baby with the 22q11.2 deletion will have a parent who also has the deletion.
Family Planning
The best time to talk about genetic risk and the availability of prenatal testing is before pregnancy. Decisions about genetic testing of at-risk asymptomatic family members are best made before pregnancy too.
DNA Banking
DNA banking is the storage of DNA (typically extracted from white blood cells) for possible future use. Because it is likely that testing methods and our understanding of genetics will improve in the future, DNA banking of affected individuals may be important. See Image testing.jpg for a list of laboratories offering DNA banking.
Prenatal Testing
High-Risk Pregnancies
There are multiple reasons a pregnancy could be high-risk for the 22q11.2 deletion. This includes:
- A parent or siblings diagnosed with the 22q11.2 deletion
- Prenatal screening test, like NIPT, with a high-risk result
- Ultrasound that identifies birth defects, like a heart problem, that are associated with the 22q11.2 deletion. Some types of heart problems called conotruncal cardiac anomalies: interrupted aortic arch, truncus arteriosus, tetralogy of Fallot, and ventricular septal defect (VSD) are seen in fetus’ with the 22q11.2 deletion
In high-risk pregnancies, genetic testing is available either during the pregnancy or after the baby is born. Testing done during a pregnancy or prenatal testing requires an invasive procedure, either an amniocentesis usually performed at 15-18 weeks’ gestation or a CVS performed at 10-12 weeks’ gestation. A prenatal test uses the same testing methods described in Molecular Genetic Testing to diagnosis the 22q11.2 deletion.
Fetuses at increased risk for the 22q11.2 deletion may have extra screening tests done between 18-22 weeks’ gestation including a high-resolution ultrasound examination for palate differences and other associated findings or a fetal echocardiograph (echo) for heart problems.
Low-Risk Pregnancies
Non-invasive prenatal testing (NIPT) is a screening test done on a maternal blood sample to analyze placental cell-free DNA (cfDNA) and determine the chance that a fetus has specific genetic conditions. NIPT can detect common trisomies (like Trisomy 21 or Down syndrome), and also select microdeletion syndromes including the 22q11.2 deletion syndrome. The accuracy of NIPT for the 22q11.2 deletion and the ability to detect different sized deletions varies based on the testing method used. SNP based NIPT is the most accurate testing method and recently has been shown to detect deletions smaller than the typical 3 Mb deletion. Pregnancies found to be high-risk for the 22q11.2 deletion by NIPT need confirmatory diagnostic testing.
Knowing about a diagnosis or suspected diagnosis of the 22q11.2 deletion syndrome, even late in pregnancy, can be useful for medical management after the baby is born.
Note: Gestational age is expressed as menstrual weeks calculated either from the first day of the last normal menstrual period or by ultrasound measurements.